Neurology is a unique field because there are so many subspecialties within it that are vastly different from one another! Neurology residency is 3 years of training after a preliminary internship in internal medicine. There is just no way to learn all of neurology in 3 years, and this is why there are numerous fellowships after neurology residency. After neurology residency, we can train further in stroke, neurocritical care, neuromuscular/EMG, movement disorders, cognitive neurology, epilepsy/EEG, neuro-oncology, sleep, autoimmune/immunology, MS, neuro-infectious disease, just to name a few! I am personally doing neurocritical care fellowship after neurology residency. I will share with you my experience as a neurology resident in the largest program in the USA.
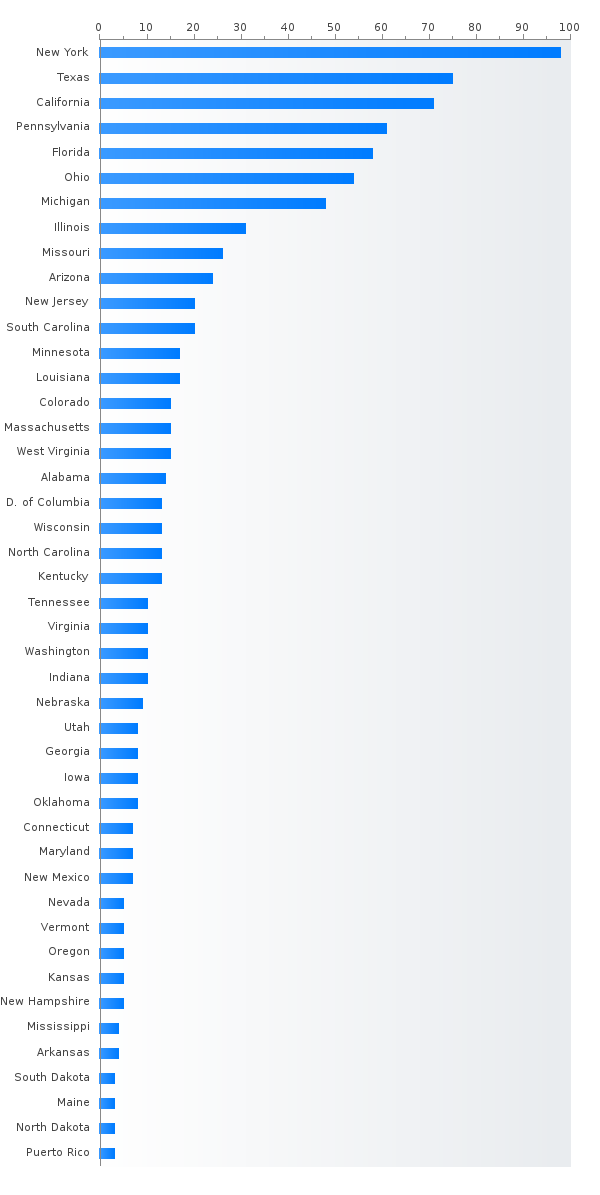
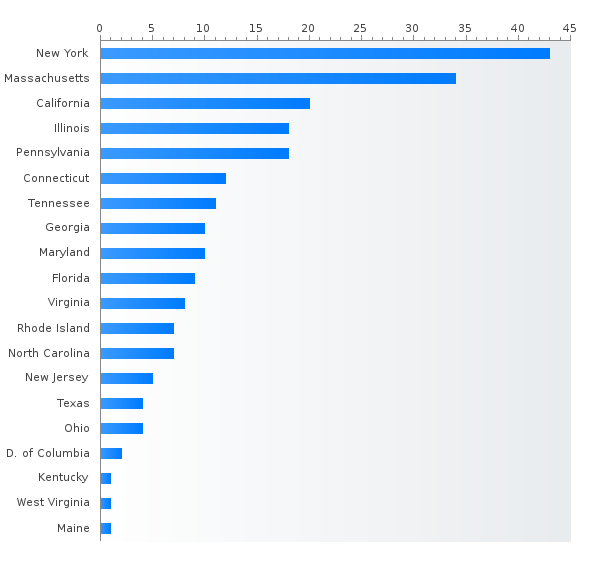
My residency program has about 18 residents per year, and we are divided among two very large tertiary care academic centers in Boston, with each hospital almost having 1,000 inpatient beds. For this reason, we have a very high volume of patients that we take care of, which is great for learning. When I moved from my medical school at UC San Diego to my neurology residency program in Boston, I was shocked to learn how many teams we have in comparison to where I learned neurology as a medical student. We have an inpatient stroke team, general neurology team, Emergency department consult service, general inpatient consult service, stroke and critical care consult service, neurocritical care unit, pediatric neurology consult service, and neuro-oncology primary service. That’s 8 neurology teams at any given time in the hospital. While there are advantages to having such a large patient volume and group of attendings to learn from, there certainly is less of a “small family” feel to my residency program, as we don’t have a lot of one-on-one time with the same faculty members. However, our program tries to mitigate this by having small groups, or “houses” where the residents are divided with faculty advisors. It is still a self-motivated type of program, though. Smaller programs may have more hands-on mentorship and so called “hand-holding” than my program does! I love having a group of co-residents with such different backgrounds and interests, though. Everyone seems to find their own niche!
My favorite part of neurology residency has been the steep learning curve I experienced as a first year neurology resident (or PGY-2) and how I felt immense academic growth during that year. It was a high-volume, high work load year for me, but I learned the most as a neurologist in that year. The subsequent years (PGY3 and PGY4) were more of learning leadership skills, management skills and supervising others as a senior resident. This was also fun, but nothing like the intensity of PGY-2 year
The biggest challenge of neurology residency, in my opinion, is learning enough outpatient neurology to be able to feel competent as a general neurologist. This is because most neurology residencies are heavily inpatient weighted, meaning we see a lot of acute stroke, seizures, and other emergencies. We don’t always get as familiar with clinic neurology. The second biggest challenge is that there is so much to learn within neurology, and residency is almost like the tip of the iceberg! There is a wealth of knowledge to be gained within all the subspecialties of neurology that only comes with time and experience.
My advice to anyone applying to neurology residency is to keep an open mind about what you want to do after residency in terms of fellowship. Many people change their mind and interests once they start neurology residency. I also recommend choosing a program that feels like it’s the right fit for you, especially when it come to the size of the program because this determines how much mentorship you will have from program leadership and your attendings. Lastly, choose a program with a high volume of patients and consults to maximize your exposure during residency. Neurology residency is a challenging but ultimately very rewarding time!
Read more